Nowadays, oral health issues have become one of the significant challenges in global public health. Poor oral care can lead to a series of problems such as dental caries (cavities), periodontal disease, mouth ulcers, and dental malformations. This guide will introduce the importance of oral care, the categories of oral care products, and factors influencing consumers' choices of oral care products, helping you make informed decisions to meet your diverse needs.
Oral Health Issues and Oral Care
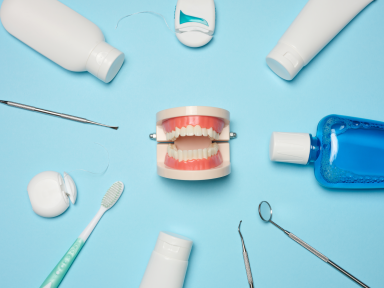
Oral Health Issues and Oral Care
Mouth Ulcer
Oral ulcers are usually easy to identify. They appear as white patches on the gums, tongue, inner cheeks, inner lips, or the roof of the mouth. There are various causes of oral ulcers, such as accidental bites, vitamin deficiencies, oral diseases, or orthodontic care. Maintaining oral hygiene and a healthy diet can help prevent them. Most importantly, using effective oral ulcer medications correctly during treatment is essential, such as Ulceloocin oral or ulce patch
Tooth Decay
Tooth decay is caused by the buildup of dental plaque, which produces acids that erode tooth enamel, leading to visible black spots. To prevent cavities, it is recommended to use antibacterial mouthwash appropriately in addition to daily brushing and to limit the intake of sugary foods and drinks.
Periodontal Disease
Periodontal disease, or gum inflammation, is caused by dental plaque, diabetes, or pregnancy. If not prevented and treated promptly, it can lead to tooth loss. Maintaining oral hygiene and regular health check-ups are effective ways to prevent periodontal disease.
Malocclusion
Malocclusion can affect biting function and facial aesthetics, so wearing orthodontic appliances correctly is essential to address misaligned teeth. During the treatment, it's important not only to maintain oral hygiene but also to clean the aligners regularly with specialized cleaning tablets. Additionally, since the sharp edges of the appliances may repeatedly irritate the oral mucosa—especially during the initial adjustment period—traumatic oral ulcers can easily occur. Therefore, it’s advisable to keep effective oral ulcer patches or sprays on hand.
Oral Care Product Category
Scientific selection of oral care products is of great significance for maintaining oral health, preventing diseases, and optimizing quality of life. Different oral issues require targeted oral care products, each with its own advantages and disadvantages, necessitating proper and rational use.
Oral Ulcer Spray

Ingredients include:
Antibacterial and anti-inflammatory ingredients: Hydrogen peroxide, Povidone iodine
Natural extracts: Honeysuckle, Propolis, Menthol, Borneol, etc.
Vitamins: Vitamin B
The oral ulcer spray is portable and easy to use, offering a more comfortable experience compared to oral ulcer patches without any foreign body sensation. However, its effectiveness is limited, and it may not precisely cover the wound.
Dental Care Products for Cavities
Electric Toothbrush

Clinical studies show that proper use of an electric toothbrush can reduce the incidence of cavities by 21% and the risk of gingivitis by 42%. Compared to other oral hygiene products, sonic toothbrushes utilize high-speed vibrations to create dynamic and fluid movements, effectively cleaning between teeth and removing plaque.
Toothpaste

Fluoride toothpaste is essential for preventing cavities as it strengthens tooth enamel and helps ward off decay. Whitening toothpaste contains mild abrasives that remove surface stains and brighten teeth. However, not all toothpastes aid in preventing cavities and whitening; some may cause tooth sensitivity or increase the risk of cavities.
Antibacterial mouthwash

Therapeutic mouthwash contains active ingredients such as fluoride, preservatives, or antimicrobial agents, which help reduce plaque, prevent cavities, and treat gum disease. However, excessive use can lead to mouth ulcers, so it is advised not to rely on it too heavily.
Orthodontic Care Products
Oral Ulcer Patch
During the initial adaptation phase, friction between the orthodontic appliance and the oral mucosa can easily cause traumatic oral ulcers. Therefore, oral ulcer patches are one of the essential products for orthodontic care.
Interdental Brushes

Interdental brushes are small tools specifically designed for cleaning the gaps between teeth that regular toothbrushes cannot thoroughly reach. They come in various sizes to fit different gaps and are ideal for people with braces or dental bridges.
Retainer Cleaning Tablets
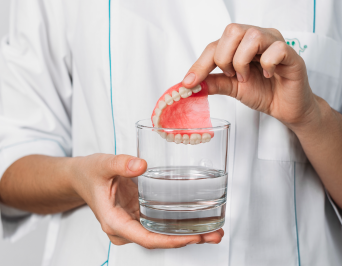
Retainer cleaning tablets can effectively remove bacteria, stains, food residue, and odors from the retainer's surface, keeping it clean and hygienic while extending its lifespan.
Factors Influencing Consumers' Choice of Oral Care Products
There are many types of oral care products on the market, and how consumers choose the right oral care product is a major challenge. Consumers' selection of oral care products depends on the following factors:
1. Price, Supply, and Packaging of Oral Care Products.
For oral care products, due to their high frequency of use, consumers are more inclined to choose cost-effective, affordable, and practical products.
2. Consumer Income.
The higher the consumer's income, the more they pursue a high-quality lifestyle. As a result, they often place greater emphasis on oral care products, with higher demands for such products. Compared to price, they prioritize the quality and effectiveness of the products.
3. Personal Awareness and Habits.
The choice of oral care products also depends on personal lifestyle habits and awareness. Each consumer has different habits regarding the use of oral care products, leading to variations in the products they purchase and the quantities they buy. For example, approximately 60%-70% of consumers prefer purchasing oral ulcer patches over oral ulcer sprays, as they believe the patches are more convenient and effective. Meanwhile, 30%-40% of consumers buy mouthwash due to their daily habits.
How to Choose the Best Oral Care Products
Choosing the best oral care products not only boosts profits but also enhances customer satisfaction. The following factors can help you make the best selection.
Professional Qualifications of the Product
To meet consumer needs, purchase oral care products with professional qualifications to gain their trust. For example, when selecting anti-cavity oral care products, look for fluoride toothpaste and mouthwash that carry the American Dental Association (ADA) Seal of Acceptance.
Anti-Allergy Effect
For consumers with allergy symptoms, using natural or hypoallergenic products, such as Tom's of Maine fluoride-free toothpaste or Hello Sensitivity Relief fluoride toothpaste, may be helpful. Always check the ingredient list before purchasing to avoid potential allergens.
Price and Availability
Supplying and procuring cost-effective oral care products is the right choice. At the same time, it should be noted that consumer groups with different incomes have varying levels of price sensitivity toward oral care products. Therefore, it is possible to recommend products at different price points to cater to the needs of various consumer groups.
Differentiated Products Under Personalized Demands
Understanding consumers' personalized needs and selecting differentiated products, such as functional differentiation or design differentiation, helps enhance competitiveness and consumer satisfaction.
Environmental Sustainability
For environmentally conscious consumers, the sustainability of oral hygiene products is an important factor. Look for toothbrushes made from biodegradable materials, such as bamboo toothbrushes like Brush with Bamboo or The Humble Co.
Conclusion
The scientific selection of oral care products is not only the core of consumer health management but also the key for suppliers to enhance product competitiveness and market trust. In the future, with technological innovations and the rise of personalized consumer demands, more opportunities and challenges will emerge.






















